What is Carprofen For Dogs?
Carprofen for dogs is a prescription medication that is a non-steroidal anti-inflammatory drug (NSAID) that provides moderate relief from pain and reduces inflammation. It is likely available at your animal hospital and is one of the most commonly prescribed pain medications in veterinary medicine.
It is available in both tablet and injectable forms. Carprofen comes in multiple brand names including Rimadyl®, Rimifin®, Carpox®, Tergive®, Carprodyl®, Carprieve®, Norocarp®, Novox®, quellin®, Rovera®, and Vetprofen®.
What is Carprofen Used For in Dogs?
Carprofen for dogs is used in veterinary medicine to relieve moderate pain and inflammation associated with osteoarthritis and postoperative soft tissue and orthopedic pain. Osteoarthritis results in pain, stiffness, and lameness and is the number 1 cause of chronic pain in dogs in the United States.
While it is most commonly seen in older dogs due to wear and tear on the joints, it is occasionally seen in younger patients. This is especially true for dogs that have a developmental orthopedic disease like hip and elbow dysplasia.
Is Carprofen Safe For Dogs?
As with any other medication, there is always a small risk of adverse effects. Carprofen should be used with great caution in dogs younger than six weeks of age, dogs with hepatic or kidney disease, pregnant or lactating dogs, dehydrated animals, or dogs with gastrointestinal upset. It is essential to always consult with a veterinarian before administering Carprofen to a dog.
How Does Carprofen For Dogs Work?
Most conditions that cause pain have an inflammatory component. To understand how Carprofen works, we first need to understand the cascade of events that occur with inflammation.
There is a complex interaction between proteins and enzymes that either activate or deactivate one another. Cyclooxygenase enzymes (COX) are a group of enzymes that play a pivotal role in inflammation and pain.
They coordinate in a balanced way to regulate the body’s normal homeostasis and are upregulated in response to tissue or bone trauma. When activated (especially COX-2), they stimulate the release of inflammatory mediators; prostaglandins, thromboxane, and leukotrienes.
Inflammatory prostaglandins play a pivotal role in inflammation, both at the injury site and in the brain. Carprofen is a non-steroidal, non-narcotic anti-inflammatory drug that works by inhibiting COX enzymes. This puts the breaks on the inflammatory cascade, and therefore relief of pain.
Recommended Dosages of Carprofen in Dogs
| Weight (Lbs) | Weight (Kg) | Tablet Size | Daily dosage |
| 5-10 | 2.3-4.5 | 25mg | 1/2 |
| 11-15 | 5-6.8 | 25mg | 1 |
| 16-20 | 7.3-9 | 75mg | 1/2 |
| 21-30 | 9.5-13.6 | 100mg | 1/2 |
| 31-40 | 14-18.2 | 75mg | 1 |
| 41-60 | 18.6-27.3 | 100mg | 1 |
| 61-90 | 27.7-40.1 | 100mg | 1 1/2 |
| 91-120 | 41.4-55 | 100mg | 2 |
Using Carprofen With Adjunctive Agents
Carprofen for dogs is highly effective at controlling mild and moderate pain. Occasionally more needs to be done to control severe pain. Furthermore, the addition of adjunctive agents may allow for a dose reduction in Carprofen or provide an alternative if the dog is sensitive to the effects of Carprofen.
Depending on the type of pain, many modalities can be applied to provide pain relief. Additional pharmacological agents offer an option for both short-term and long-term drug therapy. Physical therapy, weight control, acupuncture, and nutraceuticals provide drug-free options for the management of pain. These are discussed further below:
Pharmacological Agents
Chronic pain is characterized as the type of pain that will not abate with rest and tissue healing. This type of pain has a terrible effect on a pet’s quality of life and thus requires treatment. Unfortunately, there are circumstances when carprofen alone does not provide a dog with adequate pain relief.
Another circumstance often seen is that the dog responds to carprofen for a period, but as tissue and joint trauma progress, the need for adjunctive pharmacological agents increases. However, before discussing additional pharmacological agents used to control chronic pain in dogs, we first need to understand the types of pain involved. These can be loosely categorized into two major groups: inflammatory pain and neuropathic pain.
Inflammatory Pain
As already mentioned, inflammatory pain is what is targeted by carprofen. It is the most common component of most types of pain. While Carprofen is very effective at controlling inflammatory pain, it does not control other kinds of pain.
Neuropathic Pain
Neuropathic pain is a different type of pain. It is maladaptive and intense. It occurs as a result of “overactive” pain pathways. It can lead to an exaggerated pain response. Common examples of this type of pain include nerve entrapment or damage, lumbosacral disk disease, feline lower urinary tract disease, and osteoarthritis.
The drug Gabapentin is often prescribed by veterinarians to address neuropathic pain.
Gabapentin
Gabapentin is a drug approved for use in humans for the management of seizures and certain pain conditions. Its use is off-label in veterinary medicine for the control of pain. It acts on nerves to inhibit the release of neurotransmitters involved in the sensation of pain.

Dose and administration frequency will vary significantly between individual pets and may need to be adjusted based on response. Dosing starts as low as 5mg/kg twice daily but may go as high as 20mg/kg three times daily. Mild sedation is reported in some dogs, but this can often be alleviated using a lower dose.
Amantadine
Amantadine is an antiviral drug that coincidentally has been found to contribute to pain relief by blocking receptors in the pain pathway of the central nervous system. It is used as part of a multimodal protocol for pain control at a dose of 3-5mg/kg once to twice daily.
Corticosteroids
This group of hormone-based drugs has potent anti-inflammatory properties. Most prescribed forms include prednisone, prednisolone, dexamethasone, and triamcinolone. Corticosteroids suppress many inflammatory genes responsible for inflammation and, therefore, pain.
Common initial side effects observed with corticosteroid use include increased thirst and urination, increased hunger, panting, and lethargy. Long-term use can come with a plethora of more severe side effects such as increased susceptibility to infections, muscle wasting, and endocrine disease such as diabetes and Cushing’s disease.
The most important thing to note with corticosteroids is that they generally cannot be given concurrently with Carprofen (or any other NSAID). The risk of toxicity is increased when these drugs are given together.
It is essential to inform your veterinarian if your dog is receiving either of these medications so that your veterinarian can prescribe appropriately.
Physical Therapy
Physical therapy reduces pain and aids physical function and movement. It encompasses joint mobilization, massage, passage range of motion, and stretching. All of these activities work to improve muscle strength and joint fluidity.
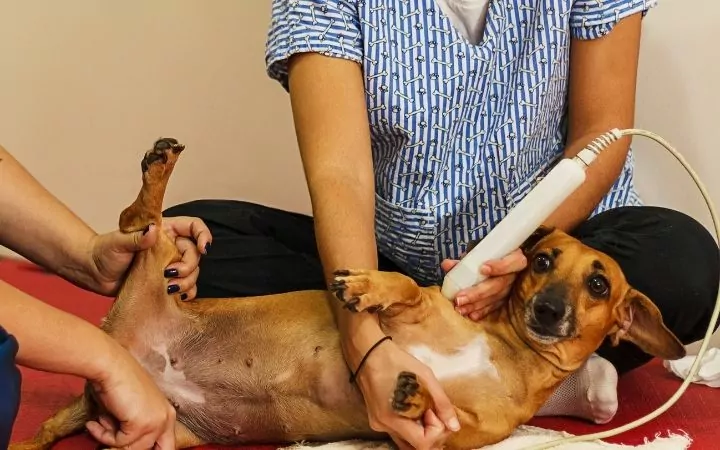
Often, physical therapy incorporates therapeutic modalities, all of which work to decrease inflammation, improve healing, modulate nerve transmission, and improve blood flow. These modalities can be discussed with your veterinarian. These modalities include:
- Cryotherapy (icing)
- Thermotherapy (heat packs)
- Extracorporeal shock wave therapy
- Laser
- Pulsed electromagnetic field (PEMF)
- Transcutaneous electrical nerve stimulation (TENS)
Exercise and Weight Control
Ensuring your dog is not overweight is pivotal to the management of many chronic pain conditions. Increased body mass places increased load on the body’s joints and can have severe consequences for dogs with conditions such as hip dysplasia, elbow dysplasia, or osteoarthritis.
Low impact and high resistance exercises such as swimming help build muscle and strength while supporting the dog’s weight. If you don’t have access to a hydrotherapy pool or any other water source, then that’s ok too. Going for gentle regular walks will achieve the same goal.
Exercise is only part of the equation when it comes to addressing weight control. Diet is the primary determinant of body weight, and many pets with chronic pain conditions are overweight. Consult your veterinarian to determine if your pet is obese.
It can be difficult for owners to limit their pets’ food intake for logistical, emotional, or practical reasons. Feeding guidelines on pet food packages can often be overly generous, and like many people, dogs vary in their caloric requirements.
Regular weigh-ins and monitoring food intake, including treats, is the first step to reducing your dog’s body weight. Veterinary prescription diets are formulated to keep your dog feeling full for longer while reducing the overall caloric intake.
Acupuncture
Acupuncture works by stimulating nerves, increasing blood circulation, modulating hormone release, and decreasing muscle spasms. It is a non-pharmacological method of pain relief that is gaining increased exposure in veterinary medicine.
It is most commonly used for patients with chronic pain conditions such as osteoarthritis, hip dysplasia, intervertebral disk disease, or other spinal conditions. Thus, acupuncture is an ideal adjunct to pharmacological treatment of pain conditions.
Nutraceuticals and Supplements
Nutraceuticals are biological therapies derived from foods containing bioactive ingredients that have physiological benefits and aid in treating and preventing medical conditions. These include supplements that contain omega-3 fatty acids, glucosamine, and antioxidants.
It is important to note that supplements for the pet industry are not regulated, and quality can vary markedly from one manufacturer to another. It is recommended to stick with brands recommended by veterinarians because these generally come from trusted manufacturers.
Known Side Effects of Carprofen in Canines
The incidence of side effects associated with the use of NSAIDs like carprofen is unknown but is believed to be very low. The most common side effects result from gastrointestinal upset, renal toxicity (kidney toxicity), and liver toxicity.
Gastrointestinal Toxicity
Gastrointestinal ulceration is the most common side effect of carprofen use. Because we cannot “see” gastrointestinal ulceration directly, it is pivotal that owners monitor for evidence of gastrointestinal ulceration.
Signs to look out for include depression, inappetence, vomiting, diarrhea, and tarry or bloody stool. If any of these signs are seen, carprofen should be immediately discontinued, and a veterinarian should be consulted.
Renal Toxicity
COX enzymes play an important role in normal kidney functions, but the exact mechanism in which carprofen can cause renal toxicity is not fully understood. It is believed that prostaglandins are responsible for the maintenance of renal blood flow.
NSAIDs prevent prostaglandin release and reduce blood flow and oxygenation to the kidneys, resulting in tissue hypoxia and death. Therefore, dogs should be screened for evidence of underlying renal insufficiency before starting carprofen because dogs with underlying kidney disease are most at risk of carprofen-induced kidney damage.
Liver Toxicity
The liver processes all NSAIDs. The rate of carprofen-induced liver damage is low. Most NSAID-induced side effects that affect the liver occur within three weeks of starting therapy. Consultation with a veterinarian is essential to ensure that liver function is monitored at a frequency that ensures minimal effects on liver function.
Some strategies can help prevent side effects. First, it is crucial always to communicate all currently administered medications when consulting with your veterinarian. This allows the veterinarian to avoid concurrent use of NSAIDS with drugs that are not compatible.
Your veterinarian can also help determine if your dog is an appropriate candidate for Carporfen therapy. For example, it should be avoided or used with caution in patients with renal, cardiac, or hepatic disease.
Many of our pets have underlying liver or kidney impairment but show no outward clinical signs. This is why it is important to have blood work performed. Bloodwork is an indirect measure of liver, kidney, and blood cell health.
Before starting therapy, all animals should be screened for underlying medical concerns. This includes a complete physical examination and blood work to assess hematological and chemistry parameters.
The frequency at which blood work is performed for ongoing monitoring depends on the individual dog. However, on the rare occasion that side effects occur, they most commonly occur between two and four weeks after the start of treatment.
For this reason, blood work should be repeated two-four weeks after starting carprofen therapy. In an otherwise healthy dog, blood work may be repeated every six-12 weeks.
Dogs considered “at-risk” might have blood work performed as frequently as every two to four months. However, there is no clear consensus on how often blood work should be repeated.
In addition to blood work, monitoring clinical signs of side effects is a good way to catch things early. In addition to what has already been mentioned, things to look out for include increased water consumption, increased urination, yellow or pale gums, or odd behavioral changes.
Carprofen vs. Ibuprofen for Dogs
Not all NSAIDs are the same, and dogs are not small people. For example, Ibuprofen is an NSAID commonly used in humans for the management of pain and fever. It is available over the counter in either tablet or liquid form. Common brand names include Advil, Midol, or Motrin.
In humans, Ibuprofen has a wide safety margin, and very rarely are side effects observed. This is not the case with our pets. When Ibuprofen is given to pets, the risk of toxicity is very high, and the Animal Poison Control Center reports that over-the-counter medications like Ibuprofen are the most frequently reported drug exposure reported.
If given to dogs, Ibuprofen can cause gastric ulceration, kidney failure, and liver damage. These effects may not be seen for many weeks if Ibuprofen is given at lower doses. At doses greater than 400mg/kg, dogs may seize or go into a coma. Because of its very narrow safety margin, Ibuprofen should never be given to dogs.
Treatment for ibuprofen toxicity depends on the dose, how long ago the pet took Ibuprofen, and concurrent medications or disease conditions. If your dog has been exposed to Ibuprofen, it is vital to contact a veterinarian immediately.
What is a Carprofen Substitute For Dogs?
Carprofen is not the only NSAID used for the management of pain in dogs. Other NSAIDs are available, some of which vary slightly in their mode of action. For example, previously, we mentioned that NSAIDS target COX enzymes, but there are different types of COX enzymes.
COX-1 is an important and beneficial enzyme involved in the body’s normal functions. COX-2 is induced by inflammation.
Non-selective NSAIDs inhibit both COX-1 and COX-2. Some NSAIDs, such as firocoxib, are more selective for COX-2 and, in theory, may cause fewer side effects. However, the clinical relevance of this has not been fully established.
Other NSAIDs approved for use in dogs include deracoxib (Deramaxx, Doxidyl), meloxicam (Metacam), firocoxib (Previcox), etodolac (Etogesic), ketoprofen (Ketofen, KetoMed), robenacoxib (Onsior), and grapiprant (Galliprant).
Grapiprant is a newer NSAID that was approved for use in dogs in 2016. Unlike other NSAIDs, grapiprant does not target COX enzymes. It works directly on specific prostaglandin receptors that are involved in inflammation.
While Grapiprant appears to have more selectivity, many of these prostaglandins are involved in normal homeostasis, and therefore the risk of side effects is not eliminated.
Carprofen For Dogs: At A Glance
- Carprofen is a prescription medication approved for use in dogs.
- It is a non-steroidal anti-inflammatory drug (NSAID) used in veterinary medicine to relieve moderate pain and inflammation associated with osteoarthritis, postoperative soft tissue, and orthopedic pain.
- Carprofen for dogs is highly effective at controlling mild and moderate pain.
- The incidence of side effects is unknown but is believed to be very low. The most common side effects result from gastrointestinal upset, renal toxicity (kidney toxicity), and liver toxicity.
- Carprofen should be used with great caution in dogs younger than six weeks of age, dogs with hepatic or kidney disease, pregnant or lactating dogs, dehydrated animals, or dogs with gastrointestinal upset.
- Not all NSAIDs are equal. Only use veterinary-approved NSAIDs for dogs and always do so under the guidance of a veterinarian.
