Immune-Mediated Haemolytic Anaemia. It’s a long and fancy name, often known under its abbreviation: IMHA. But which causes and symptoms hide behind the long term? Even more importantly, which treatment options are there for dogs with IMHA? Take a read below!
What is Immune-Mediated Haemolytic Anemia (IMHA)?
Immune-Mediated Haemolytic Anemia (IMHA) is an autoimmune disease. This means that the body’s immune system thinks that red blood cells in the body are foreign objects. When the immune system has decided that something is foreign, it attacks it. This is normally very beneficial, but not when it’s the body’s cells that are being attacked.
What happens when the immune system attacks the cells? The clue is actually in the name. The immune system destroys (hemolyze) the animal’s own red blood cells—this causes the animal to become anemic (low red cell count).
The immune system coats the red blood cells with antibodies – thereby targeting them for destruction. The body then lyses (destroys) the red blood cells by removing them effectively from the blood circulation.
As most people know, red blood cells are important. They’re made in the bone marrow and transport oxygen around the body to all the cells. When there aren’t enough red blood cells in circulation, not enough oxygen gets transported. Resulting in the animal becoming oxygen-deprived.
Another issue with IMHA is that the red blood cells that are being destroyed need excreting. This happens through the liver and the spleen. When too many red blood cells get destroyed simultaneously, these organs can become overwhelmed—possibly resulting in even more damages and issues.
What causes IMHA, and are Some Breeds More Prone to IMHA?
The causes of IMHA are unfortunately not well understood. But, it is known that there are two forms:
Primary IMHA
The primary form means that there are no underlying causes. It is associated with certain breeds. This also means that there seems to be a genetic component involved in the disease process. Predisposed breeds are:
- American Cocker Spaniel
- Irish Setters
- Shih Tzu
- Schnauzer
- Labrador Retriever
Secondary IMHA
Secondary IMHA is when something else (from outside the body) causes the onset of the IMHA. Anything that stimulates the immune system, can, in theory, be the cause of IMHA in a patient. This can, for example, be.
In most cases (65 – 70%), the cause is never found and is therefore idiopathic.
What are the symptoms of Immune-Mediated Hemolytic Anemia?
So what are the symptoms of this disease? There are quite a few things that happen in the body when the immune system starts destroying its blood cells. The first two things that occur are:
- Anemia. As aforementioned, the number of red blood cells becomes too low.
- Auto Agglutination. The clumping of destroyed red blood cells.
This leads to one of the two types of IMHA:
- Extravascular. This occurs when the red blood cells are destroyed within the organs of the immune system. For example, the spleen. This is the most common form.
- Intravascular. When the red blood cells are destroyed within the blood vessels.
Both types can lead to a lot of clinical signs. The most common ones are.
- Weakness and lethargy
- Tachypnea (breathing too fast)
- Jaundice (yellow discoloration of the skin and eyes)
- Anorexia (not eating enough)
- Sudden death
The severity of the symptoms can vary a lot between cases, from mild to very severe. But, in quite a few instances, if left untreated, IMHA could lead to death. Therefore, it is vital to seek veterinary assistance if you suspect your dog is suffering from IMHA.
How is IMHA diagnosed?
The symptoms of IMHA are, unfortunately, not very specific. That makes it difficult to diagnose. First, the presence of anemia needs to be confirmed. Hereafter the type of anemia is defined. Anemia can be one of two types;
- Regenerative. Where the body is stimulated to make more red blood cells. This to make up for the lost ones.
- Non-regenerative. In these cases, the bone marrow is affected. This means that the number of red blood cells isn’t regenerated.
Most often anemia is regenerative. Therefore, it is essential to rule out other causes of regenerative anemia. As well as other rare causes of hemolysis. Before getting closer to a confirmed diagnosis of IMHA.
In the end, laboratory tests are necessary to confirm a diagnosis of IMHA. This can include blood- and chemistry profiles, x-rays, urinalysis, coagulation testing, and many others. Common changes seen in blood tests in animals with IMHA include:
- Anemia
- Elevated bilirubin levels
- Increased liver enzymes
- Low PCV and HCT values (indicated a low relative amount of red blood cells in the blood)
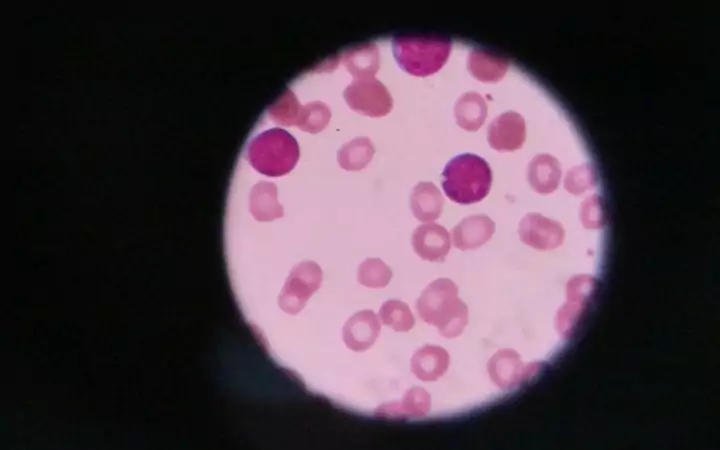
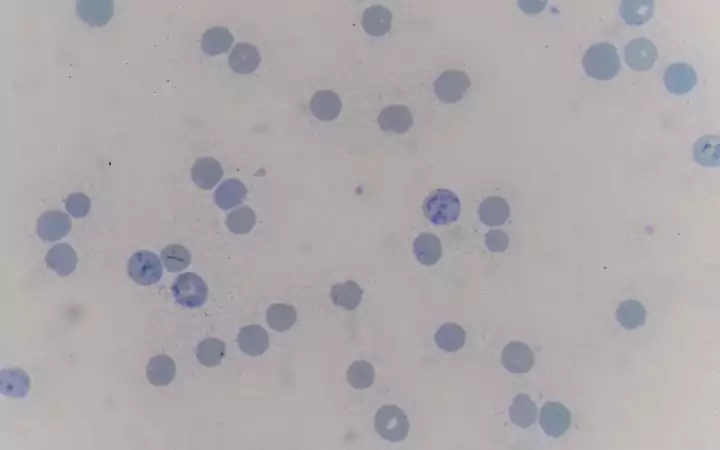
Often the blood is also examined under a microscope. Here a veterinarian will especially look for spherocytes. These are small round blood cells, which are often associated with IMHA. Reticulocytes (immature red blood cells) are also examined.
Lastly, a Coombs’ test can also be done. This test evaluates the immune response against red blood cells. A positive Coombs’ test means that there are antibodies attached to the red blood cells. This can be an excellent indicator of IMHA. It is, however, not perfect and should not be considered as the gold standard.
What treatment options are available for IMHA?
Always consult a veterinary professional before starting any kind of treatment. IMHA is – despite its seriousness – considered treatable. But, aggressive treatment is almost always needed. Treatment aims at three goals –
Remove the cause
Most IMHA causes are idiopathic, meaning a cause isn’t confirmed. But in some cases, a cause can be found, and this can be treated or at least avoided in the future. For example, if a vaccine causes the IMHA, administration of this should not happen again.
Stop the immune reaction
The first-line treatment for most autoimmune reactions is a drug called prednisolone. This is a corticosteroid that suppresses the immune system. This limits the immune response against the red blood cells, lessening the lyses of them.
If this isn’t successful, other immune-suppressing drugs can be tried. As a last resort, there is the removal of the spleen. This is very risky, and many pet owners should, at this stage, consider euthanasia as an alternative.
Often immunosuppressive medication is also a key part of the long-term plan. Animals will most often be on medication for up to 8 months after the first time of presentation. Some will be for the rest of their lives.
Provide supporting care
Besides stopping the immune reaction, most patients will also need intensive supportive care. Blood clot formation must be prevented with medication. Also, anemia often requires treatment with blood transfusion therapy. Note, though, that blood transfusion may worsen the symptoms if the new cells are destroyed too quickly.
In many cases, oxygen and fluid therapy are also used during the acute presentation of the disease. Other clinical signs can also be symptomatically treated; this includes vomiting, diarrhea, etc.
IMHA is a very complex and variable disease. This means that the treatment plan needs to be tailored to each unique patient’s needs and disease presentation.
IMHA is also notorious for causing secondary conditions in patients. The lack of oxygen due to anemia can damage the internal organs like the liver and kidneys. The most common complication, however, is the thromboembolic disease. This is when blood clots form. This can cause respiratory difficulties, sudden death, or other severe changes. So the patient should always be monitored closely.
An essential part of treating IMHA is also owner compliance. IMHA is a severe and challenging disease to deal with. In most cases, it will take extended hospital stays and continuous long-term monitoring. As well as long-term medication. It is, therefore, essential to inform the owner about the process and prognosis.
What is the prognosis with IMHA?
But what is the prognosis then? Despite the seriousness of the condition, it does carry a fair prognosis in most cases. With survival rates between 50 – 70%.
The biggest worry is often the complications caused by IMHA. For example, if the thromboembolic disease occurs, the survival rates drop significantly. But, the good news is that if the dogs do well during acute illness and treatment? They will often do well long-term.
Some patients will require life-long therapy. But, there are the patients that can be weaned from them entirely as well! Regardless, patients that survive the initial acute disease often have a very excellent quality of life, which is, after all, the most important part.
Summary
Immune-mediated hemolytic anemia is a very dangerous disease for our furry friend. It can cause severe symptoms and even much worse complications. However, it can be diagnosed, and in many cases, it can be treated. So keep an eye on your four-legged best friend and patients. Then you can hopefully soon run around, living a happy and healthy life!