Histologically stomatitis in cats is compatible with a chronic immunologic or inflammatory response; however, it does not conclude the primary cause of the disease. The term ‘stoma’ refers to a small opening in the animal’s body. In medical terminology, it is used to describe the oral cavity (mouth). Stomatitis is a generally accepted term for any type of inflammation of the oral cavity. The condition can also be described as gingivostomatitis, faucitis, or lymphocytic-plasmacytic stomatitis, based on cellular infiltrate presence.
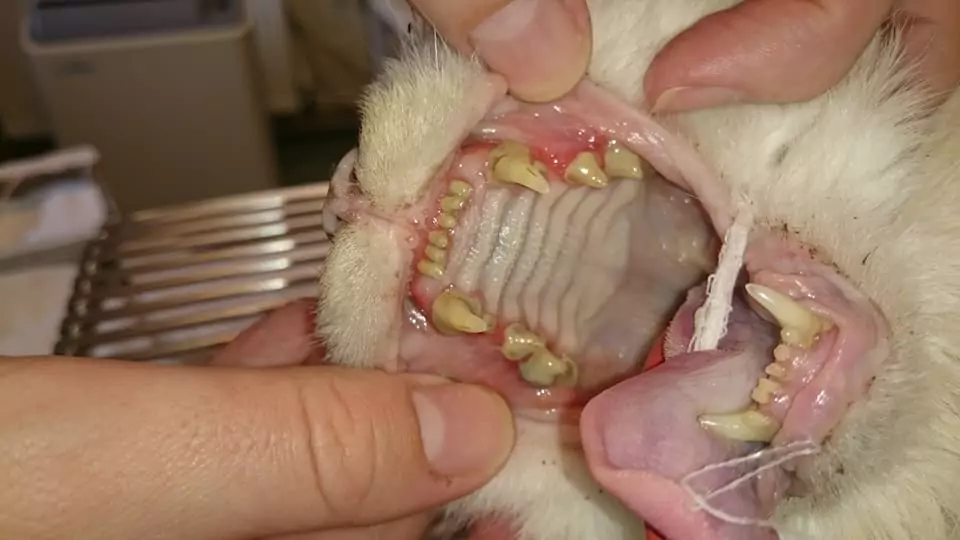
Stomatitis is widely seen in adult domestic cats, and it’s a painful and threatening problem. Purebred cats such as Somalis, Persians, and Himalayans tend to develop stomatitis at a younger age. The same goes for cats living in multi-cat households. Each case with feline stomatitis represents a great therapeutic challenge as the condition has a stubborn character.
Etiology and pathogenesis of stomatitis in cats
The etiology of stomatitis in cats remains unclear. Some data reveal that almost 90 percent of cats with chronic stomatitis were shedding both Feline Herpesvirus-1 (FHV-1) and Feline Calicivirus (FCV); Feline Immunodeficiency Virus (FIV) has been isolated from 10-80 percent of cats with stomatitis. The lowest prevalence of less than 15% has Feline Leukemia Virus (FeLV) in patients with a chronic form of stomatitis. Still, there isn’t enough information to scientifically support the correlation between any of the viruses and stomatitis in cats.
It has been suggested that stomatitis also develops due to plaque and subsequent bacteria buildup. Bacteria, however, can only play a secondary role in the pathogenesis of the condition. Plaque biofilm is associated with poor oral hygiene. When the bacteria enter the gingival sulcus (small pocket between the gums), they cause inflammation and infection.
Clinical signs of stomatitis in cats
Cats suffering from stomatitis are presented with a history of drooling, pawing at the face, bad breath (halitosis), pain upon eating, food dropping, blood-tinged saliva, weight loss, and anorexia. A significant sign is that the animals prefer soft food even if rigid food used to be their favorite treat. They become less active and can be aggressive if the owner tries to touch their face.
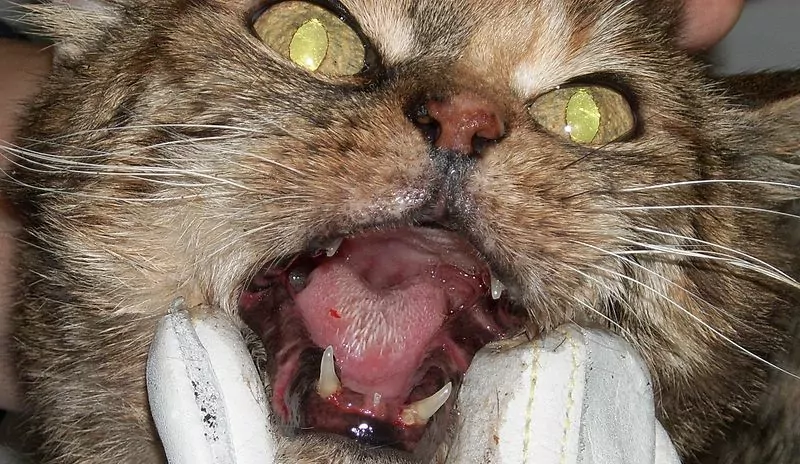
The clinical examination may reveal enlarged mandibular lymph nodes and ulcerations of the lips. Diffuse inflammation of the gingiva, buccal mucosa, alveolar mucosa, tongue, sublingual tissue, and pharynx can be noted. The cat’s hair coat will eventually become unclean and unkempt because they avoid self-grooming.
As the disease progresses, the inflamed tissue in the oral cavity takes on proliferative, raised, ulcerated, and erythematous character and tends to bleed regularly. Periodontal and dental disease of various degrees may develop, and the teeth are covered in abundant plaque.
Laboratory findings about stomatitis in cats
Veterinarians usually perform a complete blood count, biochemical evaluation of the blood, and urinalysis to identify the root of the problem. The most common findings are elevated white blood cell count, neutrophilia with a mild-left shift, monocytosis, mild lymphopenia, and eosinophilia.
Serum biochemistry reveals elevated globulins with an altered albumin/globulin ratio. Whenever possible, a serologic evaluation of FIV antibody and FeLV antigen is advisable. Virus isolation on material taken with oral swabs from the mouth can be performed but rarely helps determine the course of treatment.
A basic evaluation of the patient’s condition doesn’t include bacterial cultures. Bacterial cultures come to mind when there are chronic cases of irresponsive to antibiotic treatment. Whenever there is a neoplastic lesion of unknown cause, it’s a good idea to obtain a specimen to test for Bartonella infection.
Treatment of stomatitis in cats
The aim of the treatment protocol is to decrease the inflammatory response to the dental plaque inside the mouth. This can be achieved with brushing, topical application of antimicrobials, systemic antibiotic and anti-inflammatory therapy, laser treatment, dental scaling, and tooth removal.
Brushing the teeth of cats with stomatitis is often too difficult for owners because the animals are reacting quite painfully. In most cases, the animal will benefit from teeth scaling done by a professional under general anesthesia. After the cleaning, the gums and the teeth are washed with Chlorhexidine.
To increase poor appetite or maintain a good one, some patients can be treated with a subcutaneous or intramuscular application of methylprednisolone. Other options are oral prednisone tablets, which are unpractical because of the painful state of the cat, and transdermal application of the corticosteroid. Owners need to be advised about the possible side effects of corticosteroid therapy.

Other treatment options include oral lactoferrin, which has significant immunomodulatory and antibacterial properties, and interferon, which stimulates the immune system and is recommended in cats with stomatitis. Some reports suggest that dramatic improvement can be achieved with repeated laser CO2 treatment of the inflamed tissue in the mouth cavity.
Systematic antibiotic treatment is widely used in cases of feline stomatitis. Generally, antibiotics of choice include amoxicillin/clavulanic acid, doxycycline, metronidazole, and clindamycin. The use of Azithromycin is helpful when Bartonella is linked to oral inflammation. Unfortunately, antibiotics only provide short-term clinical improvement and can be even ineffective in alleviating the symptoms.
In cases of periodontitis and retained roots, extraction of teeth is indicated. Even healthy teeth can be extracted when the response to conservative medical treatment is poor or when the side effects associated with the medications are unacceptable.
When you extract the teeth, there is no surface where the plaque can retain. Thus the accumulation of bacteria is minimized, and the secondary inflammatory response associated with the microorganisms reduces. Most cats tolerate extractions pretty well and can eat both dry and moist food without teeth.
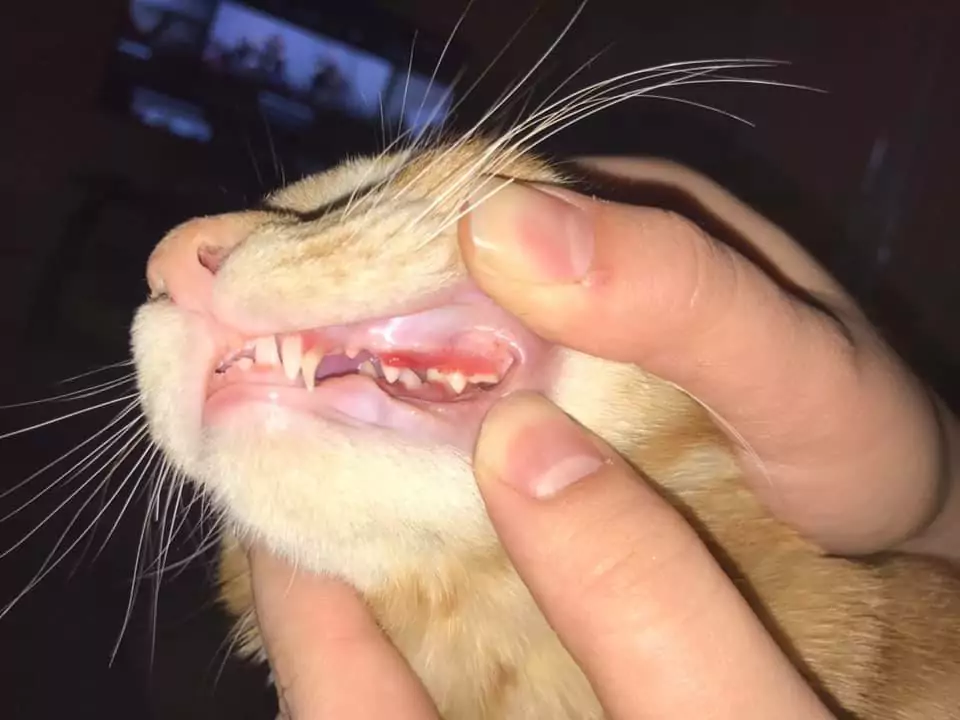
Tooth extraction is performed under general anesthesia, and before the procedure, dental radiographs must be obtained to check for periodontitis, retained roots, and feline odontoclastic resorptive lesions. As a result of intubation, often the sublingual and oropharyngeal tissues swell, and intravenous application of dexamethasone on such occasions.
Postoperative pain management can be supported by regional nerve blocks. In more than half of the cases, a tooth extraction results in complete resolution of the inflammation. In approximately 20 percent of cases, the inflammation remains minimal after the operation and further improvement requires medical therapy. No improvement after a tooth extraction is noted in less than 10 percent of cats with stomatitis.
